Extensor compartments12/29/2023 
(2012) ACSM’s Sports Medicine: A Comprehensive Review. (2010) Essential Radiology for Sports Medicine. Philadelphia : Wolters Kluwer Health/Lippincott Williams & Wilkins. (2011) The 5-minute Sports Medicine Consult. Release of the fascial sheaths of the tendons in the first dorsal compartment (doesn’t appear to be typically done)Postoperatively, the wrist is splinted for 7–10 days followed by a stretching and strengthening program, and return to sport is allowed when the patient is symptom free (3)Īuthor Dr. exploration and debridement of the intersection zone and excision of adventitial bursal tissue.release of the second dorsal compartment.Consider only after failed prolonged conservative management If the initial treatment fails after 3-4 weeks, a referral to surgery is indicated surgery is very rarely indicated. If there is insufficient improvement in pain and function al after 2-3 weeks of the above measures, consider a corticosteroid injection (mixed with local anesthetic) into the bursa or tendon sheaths as appropriate.Consider change in techniques or oar size in rowers Activity modification when returning to the aggravating sport/activity to minimize repetitive micro trauma.Referral to physiotherapy to work on stretching, ROM exercises, and strengthening of the extensor muscle groups.A short period of immobilization, for example, a thumb spica splint in 20 degrees of wrist extension may be used.A short course of anti-inflammatory medication, e.g.Rest from aggravating activities, including any repetitive forceful wrist motions.MRI is indicated if there is persistent pain despite treatment or if the diagnosis is unclear after X-rays and ultrasound An adventitial bursa between the two compartments at the level of intersection may also be seen (2) area of tenderness: may reveal tenosynovitis of tendon sheaths between the first two extensor compartments. Only indicated to rule out other pathology X-ray of the wrist and forearm: non-specific, to rule out other abnormalities not helpful in the diagnosis. Imaging is often not required for diagnosis however, imaging may help to confirm the diagnosis and/or to rule out other conditions Pain may be associated with localized swelling or crepitus (squeaking sensation) with active or resisted wrist or thumb extension (1)ĭiagnosis of intersection syndrome is based on clinical findings Pain subsides with rest from such activities 
Pain is typically worse with movements of the wrist than movements of the thumb 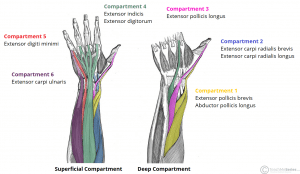
Pain worsens with activities that involve repetitive forceful wrist flexion and extension Pain is proximal to the wrist, within 4-8cm to Lister’s tubercle of the radius Patient will often present with gradual development and worsening of pain in the distal radial forearm. Extensor Carpi Ulnaris (ECU)įigure 2 – Anatomy of Intersection Syndromeįigure 3 – Surface Anatomy of Intersection Syndromeįigure 4 – Illustration of Intersection area of pain Extensor Carpi Radialis Longus and Brevis (ECRL & ECRB) 3. Abductor Pollicis Longus (APL) and Extensor Pollicis Brevis (EPB) 2. Prolonged activities that involve repetitive wrist extension and flexion increases the risk of this injury.įigure 1 – Extensor Compartments of Wrist Often found in rowers, weight lifters, and skiers. This condition is easily confused with and misdiagnosed with de Quervain’s tenosynovitis! Intersection syndrome is a chronic, overuse injury in the distal radial forearm where the tendons of the 1 st extensor compartment and the 2 nd extensor compartment cross over, resulting in bursitis or tenosynovitis of either or both tendon sheaths. Intersection Syndrome (Also known as crossover syndrome Oarsman’s wrist)
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
